Every day, our bodies are exposed to billions of viruses, bacteria, and parasites that can cause disease or even death. Fortunately, we have a powerful army of T cells, B cells, and other specialized cells that work together to protect us as part of our immune system.
T cells are a key component of the adaptive immune system, which recognizes and remembers specific pathogens. The adaptive immune system helps us form stronger and quicker attacks each time the same pathogen is encountered.
The process by which T cells become activated is fairly complicated, involving extracellular stimulatory signals between multiple cell types. In this article, we’ll keep things simple and describe the basic mechanisms of T cell activation.
Before diving into the mechanisms of activation, let’s cover the main types of T cells and their role in immunity.
Overview of T Cells
T cells are a type of white blood cell known as a lymphocyte. Lymphocytes protect our bodies against cancer cells and infected or damaged cells. T cells are one of the three main types of lymphocytes; the other types include B cells and Natural Killer cells.
T cells (also called T lymphocytes) have unique proteins called T cell receptors, or TCRs, on their surface membrane. TCRs recognize many specific antigens, which are strangers to our immune system that trigger an immune response.
Our immune system has multiple types of T cells, but we’ll describe two of the most influential players in activation: cytotoxic T cells and helper T cells.
Cytotoxic T Cells
Cytotoxic T cells are also called CD8+ T cells because of the CD8 glycoproteins on their surface. They’re constantly on the hunt for infected and cancerous cells and recognize antigens attached to a molecule called the major histocompatibility complex molecule (MHC) class I.
Most infected cells or pathogens express MHC class I and are identified by cytotoxic T cells which triggers their activation.
The ability of CD8+ T cells to recognize intracellular proteins makes them particularly important in controlling viral and intracellular bacterial infections. Upon activation, CD8+ T cells release cytotoxins (perforin and granzyme B) that initiate apoptosis, directly lysing target cells.
Through this lysis, virus and bacteria-infected cells are eradicated. CD8+ T cell-mediated lysis is highly specific, sparing nearby, noninfected cells.
Helper T Cells
Helper T cells are known as CD4+ T cells because of the CD4 glycoproteins on their cell surface. They recognize peptide fragments bound to MHC class II molecules and then become activated.
These cells also scan for foreign antigens and orchestrate immune responses to destroy pathogens by helping in the maturation of B cells, production of antibodies, and activating cytotoxic T cells and macrophages.
Furthermore, environmental cues (primarily cytokines) present during activation initiate CD4+ T cell differentiation into effector T cells and regulatory T cells (Tregs), each of which have distinct immune functions.
Now that you’ve been introduced to cytotoxic and helper T cells, it’s time to learn how they’re activated.
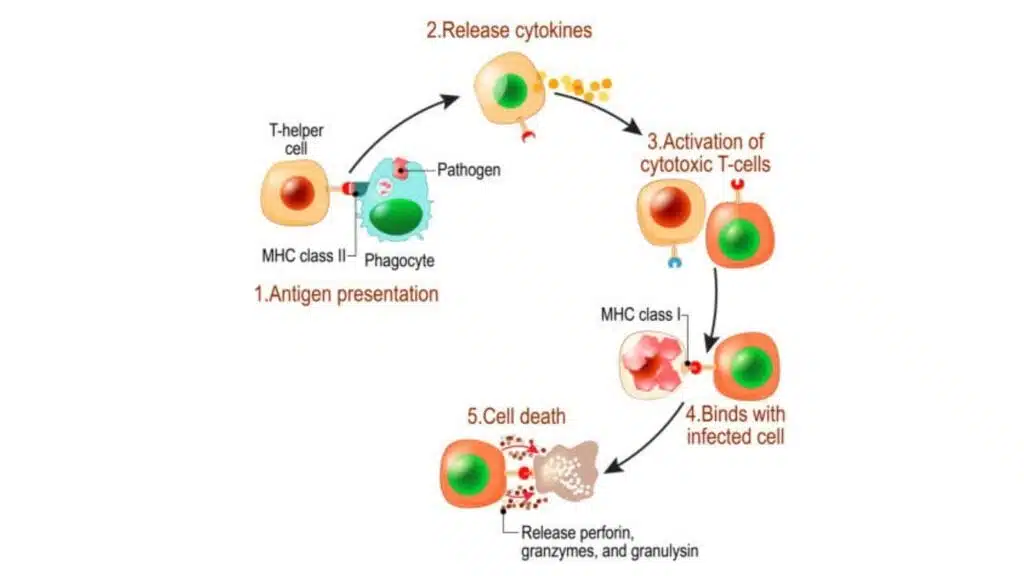
T cells are activated by the antigens they encounter in a two-signal process. Before we get into the specifics of this signaling process, it’s important to quickly look at the role of antigen presenting cells (APCs).
T Cells Activation Process
APCs are like the security guards of the human body. They’re conducting constant surveillance and detect any foreign invaders that don’t belong. Two of the most common APCs are dendritic cells and macrophages, which are phagocytic cells that simply engulf foreign particles.
The process of T cell activation begins when an APC engulfs a pathogen and its specific antigen by the process of phagocytosis. The APC digests the antigen into peptide fragments and displays these fragments to the MHC molecule on its plasma membrane.
Once the peptide antigen is present on the surface of the APC as a MHC class II peptide, the APC migrates from the site of infection to the lymph nodes where it presents to the circulating naïve helper T cells.
Just as a key fits into one lock, each T cell has a receptor that binds to only one specific antigen. This being said, if the TCR of any T cell recognizes the specific antigen MHC complex on the APC, it will bind to it. This binding is known as “signal 1” which triggers the initial activation of the T cells.
However, this alone is not enough to complete the T cell activation process. In addition to TCR binding to antigen loaded MHC, both helper and cytotoxic T cells require a number of secondary signals to become fully activated and respond to the threat. This process is known as co-stimulation.
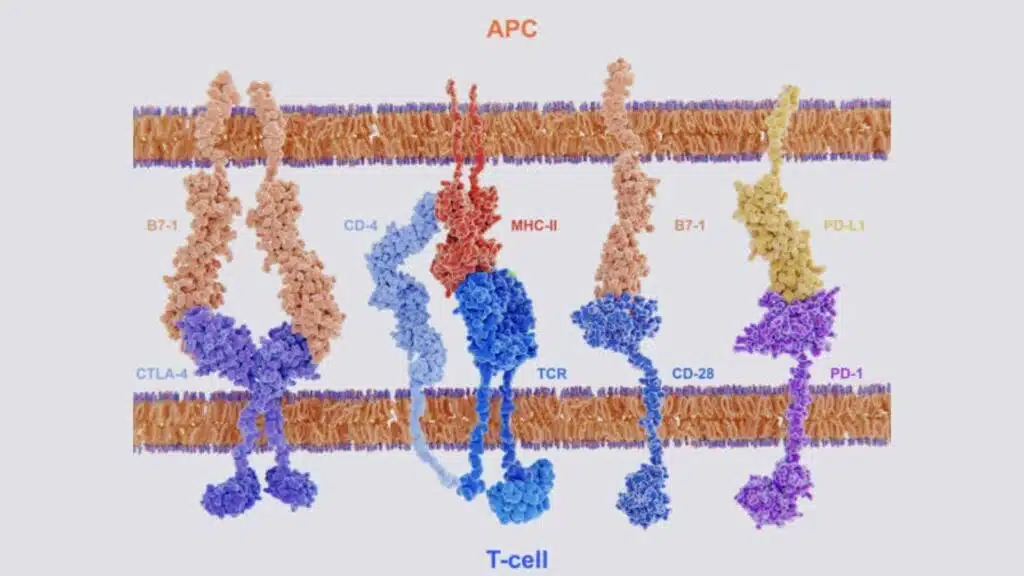
In the case of helper T cells, this second co-stimulatory signal is provided by a receptor expressed on the surface of the T cell called CD28. CD28 binds to a very important molecule on the surface of the APC called the B7 protein.
So why is this so important? Well, the binding of CD28 to B7 ensures the T cells are only activated by APCs which have encountered a pathogen and responded. Binding to B7 results in T cell activation, whereas a lack of binding results in cell death.
Thanks to the co-stimulatory CD28-B7 pair, our T cell is officially activated and the APC secretes cytokines that signal T cells to destroy the antigen. At this point, T cells undergo rapid proliferation and differentiation, and soon a population of effector T cells and memory T cells is generated.
These CD4+ effector T cells develop into diverse subsets of helper T cells and memory T cells, which have ability to quickly generate more effector T cells if the same antigen is encountered in the future
Conclusion
T cells function to actively destroy infected cells and disease, as well as to signal other immune cells to participate in the immune response.
Not surprisingly, the mechanisms of T cell activation are studied extensively by researchers focused on drug discovery, cellular therapies and vaccine development.
This article provided a brief explanation of the rather complex signaling cascade and underlying processes regulating T cell activation. New discoveries are made almost daily that are expanding our knowledge of the role T cells play in immunity, including how T cells can provide long-term protection from COVID-19.
If you’re interested in learning more on this topic, then check out some of our recent blog posts on research involving T cells and the development of new immunotherapies.