For researchers working in drug development, HLA-typed T cells are critical for investigating new immunotherapy concepts and studying disease mechanisms. In fact, T cells with HLA data are one of the most common requests we receive from our customers conducting preclinical research.
HLA, which stands for human leukocyte antigen, is a gene and protein family that contributes to immune system regulation. Due to its high diversity and immunogenicity, HLA encoded proteins play one of the most important (and often unpredictable) roles in immunology.
In this guide, we’ll cover the most common applications for T cells in preclinical research, and why researchers prefer typed cells over non-typed.
HLA Overview
Before diving into how researchers use HLA-typed T cells to develop new therapies, let’s first review how HLA encoded proteins influence an immune response.
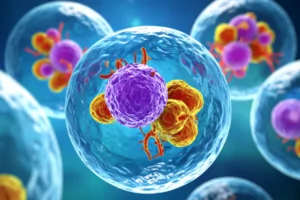
HLA plays a critical role in helping the immune system, specifically T cells, distinguish the body’s own proteins from non-self proteins made by foreign invaders (e.g., virus and bacteria).
What makes the HLA gene family truly unique compared to the rest of the coding genome is the number of unique alleles that have been identified for HLA genes.
Specifically, there are 30,522 assigned HLA alleles as of March 2021.[1] This number continues to grow as hundreds of new alleles are discovered every year.
To illustrate the relative complexity of the HLA gene family, consider the fact that the gene that determines blood type has only three possible sequence variants or alleles within the human population.[2]
HLA B is the most diverse of all human genes in the genome. This variation is known to affect susceptibility to infectious and autoimmune diseases, and therefore it is likely that this diversity contributes to donor-donor differences in primary cell experiments.
So, how do human leukocyte antigens regulate immune response?
In simple terms, HLA proteins are like serving plates containing antigenic peptides that T cells recognize as “self” or “non-self.” Once a T cell recognizes a pathogen through this HLA interaction, it begins a sequence of cell-to-cell signaling that mobilizes an immune response.
Use of HLA-typed T Cells in Research
Researchers use T cells with HLA genetic data in a wide range of applications, from basic research to the development of GMP cell manufacturing protocols.
We surveyed our customers on how they use HLA-typed T cells and identified the three common applications which we explore in greater depth below.
The most common research application by far is immuno-oncology, which broadly represents the discovery of cancer immunotherapies.
Another common application for HLA-typed T cells is the study of disease mechanisms, in particular how HLA is implicated in autoimmune disease.
Lastly, researchers use T cells with HLA data to study drug hypersensitivity and immunogenicity.
1. Immuno-oncology
Immuno-oncology (IO) is the study of the interaction of cells of the immune system with cancer cells. This scientific field has expanded rapidly in recent years due to the recent success of novel cancer immunotherapies.
IO researchers are focused on the mechanisms by which malignant cells avoid detection by the immune system, usually by breaking down presenting protein antigens at the cell surface.[3]
Current T cell receptor (TCR) and chimeric antigen receptor T cell (CAR-T cell) therapies are designed to overcome this evasion by creating artificially engineered T cells that can recognize and bind to selective tumor antigens.
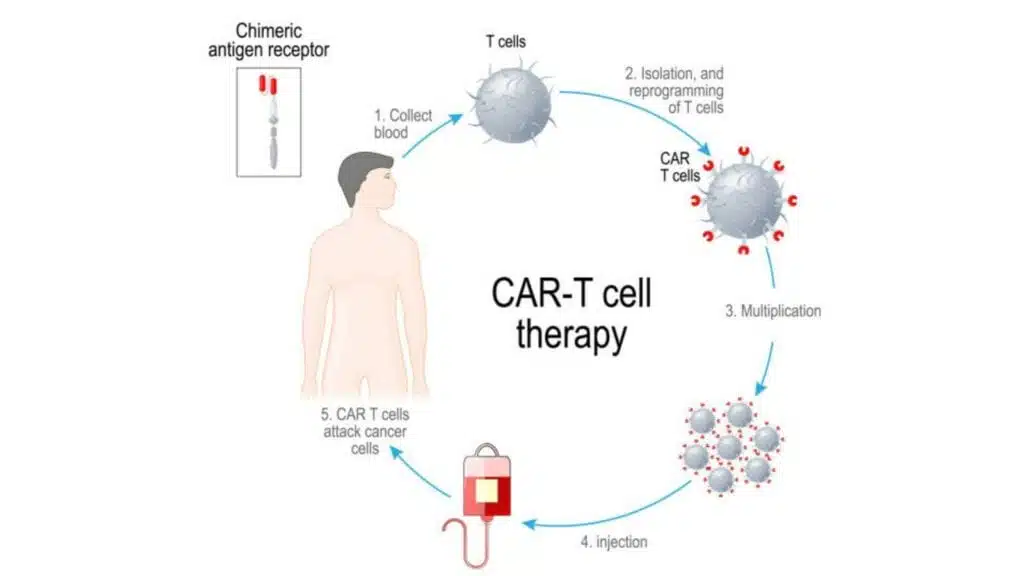
The process for manufacturing CAR-T cell therapies has 5 main steps:
- Peripheral blood mononuclear cells (PBMCs) are collected from the cancer patient through a leukapheresis procedure.
- T cells are isolated from the PBMCs, then engineered with special receptors specific for the selected tumor antigen or peptide
- The engineered T cells are multiplied in a bioreactor
- Following rigorous QC and safety testing, the engineered T cells are infused back into the patient
- The CAR-T cells kill tumor cells expressing the tumor antigen
There are currently only three FDA-approved CAR-T cell therapies, all of which are focused on treating lymphoma and leukemia. However, there are hundreds of TCR and CAR-T cell therapies currently in clinical trials or in late-stage preclinical studies with varying levels of success.[4]
So what does this all have to do with HLA?
Simply put, the success of these therapies is highly dependent upon the HLA repertoire of the patient. This is because TCR recognition is specific to both the cancer antigen and the HLA molecule presenting the peptide antigen.
Researchers developing T cell therapies must select a tumor antigen that will bind strongly to the T cell receptor as well as bind to a particular HLA allele. As described in the previous section of this post, these HLA alleles are very complicated and immensely diverse in the human population.
This begs the question, how do researchers select which HLA alleles to incorporate into the design of their TCR or CAR-T cell therapies?
The answer is that researchers usually make their section based on allele prevalence (or frequency of alleles) within a particular population or demographic.
The most frequent alleles we have identified in our donor base include HLA-A*0201 and HLA-A*0101, which are also two of the most common alleles among the U.S. population.[5]
Preclinical researchers ordering HLA-typed T cells frequently request the HLA-A*0201 allele. Not surprisingly, researchers target this allele because there will be much larger patient base eligible for the therapy upon FDA approval than if a lower frequency allele was studied.
In summary, the field of immuno-oncology encompasses many applications that require the use of HLA-specific T cells, from identifying tumor antigens to the collection and expansion of tumor antigen-specific T cells.
2. Disease Mechanisms
Another major application for HLA-specific T cells is the study of disease mechanisms or response to therapy. Plummeting sequencing prices have facilitated a significant increase in disease association studies dedicated to and identifying genomic variations associated with disease.[6]
Both Class I and Class II HLA alleles have been associated with a variety of autoimmune and infectious diseases. Accordingly, this linkage between HLA and disease constitutes biomarkers that can be used to determine an individual’s propensity for disease.
HLA polymorphisms have been correlated with disease risk, immune response to infectious disease, as well as adverse response to therapies. Certain HLA types are associated with respiratory disease, such as asthma and COPD, and also to dermatological disease such as psoriasis.[7] [8] Numerous researchers have studied the implications of HLA in facilitating disease or predicting recurrence, and our knowledge of these associations is broadening every day.
However, the functional basis for these associations is not well understood. Researchers studying the mechanisms underlying diseases, particularly autoimmune diseases, are increasingly interested in the HLA background of their primary cells.
Some researchers simply want to control their results by limiting the HLA diversity in their T cells. Others want HLA-matched T cells as healthy controls for studies and disease cells.
Such strategies by incorporating relevant genetic data into experimental design at all stages of research can only improve our understanding of donor-to-donor and thus patient-to-patient variability.

3. Drug hypersensitivity or immunogenicity
Multiple genetic and non-genetic factors can modify the action of a drug resulting in a varied response to a particular drug across different individuals. Many adverse drug reactions are caused by an unexpected immune response, often referred to as drug hypersensitivity or immunogenicity.
Genetic association studies have identified strong linkages between specific HLA Class I and II alleles and the immunogenicity of drugs, including FDA-approved therapies for gout, epilepsy and HIV.[9]
A notable example of the relationship between HLA and drug immunity is the antiretroviral drug Abacavir, which is frequently used in combination therapy to control HIV infection.
Soon after the drug was approved by the FDA in 1998, it was discovered that approximately 8% of patients taking the drug exhibited symptoms of hypersensitivity including rash, fever and gastrointestinal distress.[10]
Genetic association studies demonstrated a very strong linkage of immunogenicity in patients with the HLA-B*5701 allele. The evidence supporting a connection between HLA and hypersensitivity was so compelling that the FDA released an alert in 2008 concerning abacavir and abacavir-containing medications.
The alert recommended pre-therapy screening for HLA-B*5701 and the use of alternative therapy for patients with this allele.
Many clinical studies now implement HLA screening to prevent or limit hypersensitivity reactions due to previous drug toxicity incidents.
In addition to abacavir, there have been high-profile cases in which several monoclonal antibody therapies triggered adverse reactions among patients, including cytokine release syndrome and sepsis.
Immunogenicity screening has now become routine at every stage of therapeutic development. Preclinical and in vitro studies are incorporating HLA genetic data to screen for candidates that do not interact with high-risk HLA alleles or trigger a hypersensitivity response by any other mechanism.
Conclusion
Researchers have only begun to scratch the surface on understanding the role of HLA in treating and preventing disease. Although we described the most common uses of HLA-typed T cells in this guide, the list of applications will certainly grow as more discoveries are made in the fields of immunology, oncology and pathology.
At Cytologics, we frequently consult with customers in interpreting HLA data or understanding why a specific HLA haplotype might affect the results of their experiments. In addition, we offer a comprehensive immune cell inventory including PBMCs and isolated T cells with HLA data to support preclinical research.
If your research requires HLA-typed T cells, contact us to discuss our custom cell products collected from a diverse donor base.
References
[1] Robinson J, Halliwell JA, Hayhurst JH, Flicek P, Parham P, Marsh SGE. The IPD and IMGT/HLA database: allele variant databases. Nucleic Acids Research (2015) 43:D423-431. Accessed via http://hla.alleles.org/alleles/index.html on 2 May 2021.
[2] GB HealthWatch. ABO blood group. Accessed via https://www.gbhealthwatch.com/Trait-Blood-Type-ABO.php on 6 May 2021.
[3] Messerschmidt JL, Prendergast GC, Messerschmidt GL. How Cancers Escape Immune Destruction and Mechanisms of Action for the New Significantly Active Immune Therapies: Helping Nonimmunologists Decipher Recent Advances. Oncologist. 2016;21(2):233-243. doi:10.1634/theoncologist.2015-0282.
[4] Hildreth, C. CAR-T Cell Companies Proliferate: List of CAR-T Companies Worldwide. BioInformant. Accessed via https://bioinformant.com/car-t-companies-the-meteoric-rise-of-cellular-immunotherapies/ on 8 April 2021.
[5] Ellis, J & Henson, V & Tidwell, Rebecca & ng, Jermyn & Hartzman, Robert & Hurley, C. (2000). Frequencies of HLA-A2 alleles in five U.S. population groups. Predominance Of A02011 and identification of HLA-A0231. Human immunology. 61. 334-40.
[6] Petersen BS, Fredrich B, Hoeppner MP, Ellinghaus D, Franke A. Opportunities and challenges of whole-genome and -exome sequencing. BMC Genet. 2017;18(1):14. Published 2017 Feb 14. doi:10.1186/s12863-017-0479-5.
[7] Aralov, N & Ziyadullayev, Sh & Dushanova, Gavhar. (2020). HLA -COPD and bronchial asthma markers: commonalities and differences. International Journal of Pharmaceutical Research. 12.10.31838/ijpr/2020.12.01.202.
[8] Queiro R, Morante I, Cabezas I, Acasuso B. HLA-B27 and psoriatic disease: a modern view of an old relationship. Rheumatology, Volume 55, Issue 2. February 2016. Pages 221–229, https://doi.org/10.1093/rheumatology/kev296.
[9] Yun, J & Mattsson, J & Schnyder, K & Fontana, S & Largiader, Carlo & Yerly, Daniel. (2013). Allopurinol hypersensitivity is primarily mediated by dose-dependent oxypurinol-specific T cell response. Clinical and experimental allergy : journal of the British Society for Allergy and Clinical Immunology. 43. 1246-55. 10.1111/cea.12184.
[10] U.S. Food and Drug Administration. Abacavir Warning Bulletin, Published 2008. Accessed via https://www.accessdata.fda.gov/drugsatfda_docs/pepfar/077844PI.pdf on 5 May 2021.